“Corona” used to be such a nice word, associated with kings and fairytales, gold and gems. Nowadays it is associated with doctors and horror stories, pills, and lung ventilators.
Corona crisis is a troubling time, no doubt.
However, where a shadow is, there is also light. The pandemic has given us a lot: starting from a habit to wash our hands and up to novel business strategies. It has greatly risen the interest of the general audience towards such topics as ways of infection transmission, the mechanisms of immunity, the purpose and benefit of vaccination, and many other biology and medicine-related topics.
Now every child knows, that COVID-19 is a respiratory disease, induced by a virus, called SARS-CoV-2, that is transmitted with small droplets of saliva in the air or on objects1

However, with viruses and viral infections being “trendy”, one aspect of the pandemic remains generally overlooked. This aspect is bacterial infections and their role in our current situation.
What bacteria have to do with the Corona crisis?
Bacterial infections are the cause of many health conditions, from relatively harmless acne to deadly tetanus. These are examples of primary infections. But in the context of the current pandemic, the secondary infections are of more interest.
What is the difference?
Primary infection – a “normal” infection, caused by a pathogen in a healthy individual
Secondary infection (co-infection, superinfection) – an infection, that developed in an individual as a consequence or as a side effect of some pre-existing medical condition
For example, infection with HIV causes Acquired Immune Deficiency Syndrome (primary infection), and as a consequence of that the patient easier develops pneumonia (secondary infection)
Bacterial secondary infections were known to deteriorate the state of health in cases of viral respiratory diseases, such as influenza, for quite some time2. Recently it turned out, that the same happens in patients, infected with SARS-Cov-23. Luckily, this is not a very frequent situation – only 14,3% of the infected individuals have secondary bacterial infections as a complication of COVID-194
However, if the superinfection does happen – it increases the burden of the COVID-19 and defines the outcome of the disease. It was found out, that severity of COVID-19 of the tested patients positively correlates with the abundance of bacterial products (such as bacterial DNA and lipopolysaccharides) in their plasma5
Lipopolysaccharides – major components of the cell membrane of bacteria. They are targets of many antibiotics. Lipopolysaccharides can also be recognized by our immune cells as evidence of bacterial infection6
Secondary bacterial infections in COVID-19 patients are requiring different approaches in treatment, such as the usage of antibiotics3. All that contributes to the complexity of our current situation.
The conclusion, that we need to drive from all stated above, is that the link between anti-viral and anti-bacterial immunity is stronger than one could imagine. Understanding this link and using it to our benefit could be one of the brick stones on our road to the COVID-19 free era.
But how does our anti-bacterial immunity work? Which are the main warriors against bacterial infection? How do they protect us – and why do they harm us sometimes? How is vitamin C involved in all of this? Why is it important to supplement your body with the required amount of this vitamin to stay healthy?
Let us find out!
Important: no information, stated above, should mislead to the conclusion, that antibacterial drugs (antibiotics) are the cure from COVID-19. Antibiotics should only be taken in case of bacterial co-infection and only when prescribed by a doctor. Do not take antibiotics as self-medication or as a COVID-19 preventive measure! It will not help you and can have the opposite effect7,8
We are Neutrophils – nice to meet you!
The easiest way to meet our anti-bacterial soldiers is to squeeze out a pimple. What will you see? You will see some pus.
Sure, everybody knows, what pus is – but do you know what it consists of?
Pus is a graveyard of our immune system. Predominantly this graveyard is filled with the dead bodies of neutrophils9 – massive cells of innate immunity, which play a role of utmost importance in anti-bacterial protection. They are the reason for the yellowish color of the pus.
Neutrophils are the most abundant immune cells in the blood. Their number is 3,4 million cells per milliliter of blood in healthy males and 3,2 million in healthy females10
This makes 12-18 billion cells in the whole body!
It would not be such a shocking number, if not for that fact, that the lifespan of a neutrophil is from 5 hours to 6 days only11. So every week our set of neutrophils in blood is fully renewed. The factory producing neutrophils (same as many other white blood cells) resides in the bone marrow. Apparently, the workers of that factory never sleep or take a vacation!
But why do we need so many freshly-made neutrophils? What makes them so important?
Neutrophils are the key players of our second line of defense – innate immunity. After the first line of defense (that would be our skin) is breached by the pathogens – neutrophils are among the first warriors to start the fight. Their main role is killing bacteria, but they also take part in regulating the immune response in general and help to coordinate other cells.
So how exactly do they fight?
Actually, the human body is a house for tons of bacteria already. They live on our skin and in our digestive tract. There are more bacterial cells in our body than our own cells!12 They are good bacteria though: they help us digest our food and supplant bad bacteria. These good bacteria have evolved to peacefully coexist with(in) us and our immune system does not attack them under normal conditions. The community of good bacteria of our bodies is called the “human microbiome”
Neutrophil weapons: Phagocytosis, Degranulation and Phagocytosis
When bacteria arrive and our body and starts making a fuss, they are quickly detected by other components of our immune system. These components start signaling to their immunity-colleagues ASAP.
They scream: “Come here! It is urgent! We have an intruder!”
Neutrophils are among the first cells to respond to this call and arrive at the battlefield. The battlefield is the site of inflammation.
However, none can be considered a war hero for just arriving on the battlefield, right? Some enemy annihilation must be involved to get your medal.
How do neutrophils earn their medal?
Neutrophils have two main mechanisms of bacterial killing: phagocytosis and NETosis.
Weapon 1: Phagocytosis
Have you seen a frog catching a fly with its sticky tongue? Phagocytosis is somewhat similar to that. It is basically a process of capturing something extracellular and taking it up inside a cell. In our case, neutrophils catch bacteria, put them inside, and then digest them.
Yes, neutrophils literally eat bacteria!
However, for that to happen, bacteria first must be labeled in a specific way. This labeling is called “opsonization”. Our immune system has various instruments for labeling pathogens. One of them is well-known antibodies.
The word “phagocytosis” originates from Ancient Greek and can be translated as “eating cell”. “Opsonin” also originates from Ancient Greek and it means “preparing for eating”
How exactly does opsonization work?
Let us start by stating the obvious: bacteria are very different from human beings. This also means that molecules on the surface of bacterial cells are very different from molecules on the surface of human cells (including bacterial lipopolysaccharides, mentioned earlier). Our whole immune system is trained to detect these differences and eliminate everything that is not in our body. Well, except for microbiome residents.
Bacterial molecules, which can be recognized by the immune system as foreign, are called “antigens”. One of the approaches in fighting pathogens is the development of antibodies against these antigens. Each antibody is individually selected based on its ability to locate and bind the exact antigen. Together they form a unique perfect couple.
As soon as the antibody is developed against a specific antigen – they start to be massively produced and secreted into the blood. With the blood flow antibodies spread all over the body and locate their antigen soulmates whenever they are.
Is not that romantic? A true Antibody+Antigen love story!
However, antigens and antibodies are not the only characters in this romance. Antibodies themselves can also be recognized by the immune cells, such as neutrophils. Neutrophils have special molecules on their surface, that are sort of antibodies against antibodies.
Antigens are bound by antibodies, and antibodies are bound by neutrophils. Making a bridge between an antigen and a neutrophil is the whole purpose of opsonization.
As soon as this hierarchy is formed – neutrophils surround the bacteria with their membrane and take it up inside a cell in a special bubble, called a phagosome.
However, if we would just swallow food – it would not bring us any benefit, right? The important part is digestion!
Neutrophils are professionals when it comes to digestion!
Even before a neutrophil has encountered a bacteria – it is already full of small bubbles. These are not phagosomes, these are called granules. They are formed by neutrophils during their development. These granules are storage places of all the toxic chemicals that neutrophils use for destroying bacteria. They contain highly concentrated digestion enzymes and Reactive Oxygen Species (ROS)13
When a bacteria is internalized and a phagosome is formed, granules fuse with the phagosome to form one big bubble. In a way, that is a stomach of a neutrophil. In that stomach bacteria is exposed to all mentioned above toxic chemicals and, as a consequence, it is digested.
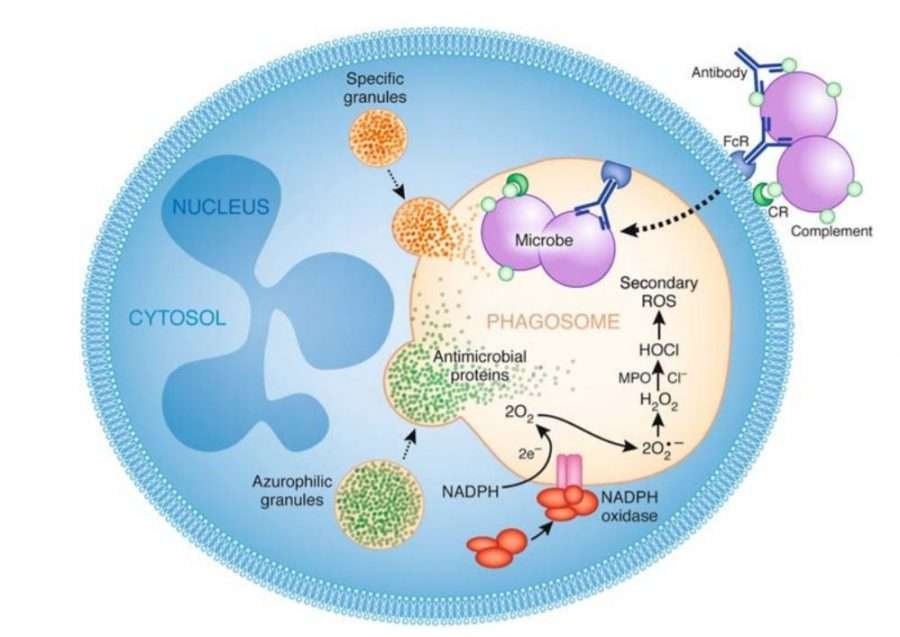
Role of Vitamin C in phagocytosis
Producing toxic chemicals is a necessity for neutrophils to carry out proper effective phagocytosis. But toxic chemicals are toxic chemicals – which means, they can be harmful to our body as well. Thus, their production and application should be tightly controlled – especially when it comes to ROS.
Our body is protected from ROS by various molecules, called antioxidants. Antioxidants interact with ROS and make them harmless. Vitamin C is one of the important antioxidants of our body, so sufficient supplementation with Vitamin C is of utmost importance15. Not only it protects us from ROS of neutrophils, but also from ROS generated by UV light.
That is not all there is to it for Vitamin C though. It has another important task!
It was shown, that Vitamin C deficiency leads to attenuated phagocytosis. There were reports of several patients with recurrent infections of the skin due to problems in neutrophil motility and function. Three patients, whose neutrophils were inefficient in bacterial killing, got supplemented with 1-2 g Vitamin C per day. As a result, the neutrophil function was restored and the health condition of the patients significantly improved16
So supplementing with Vitamin C has saved the day!
The same results were obtained in another study: patients with impaired neutrophils were supplied with 1g/day of Vitamin C for 4-6 weeks. After such treatment, the efficiency of phagocytosis was improved and matched one of the control patients, that did not have problems with neutrophils, to begin with17
Weapon 2: Degranulation
Sometimes instead of fusing granules with phagosome, neutrophils fuse granules with their cell membrane. This leads to release of antibacterial chemical compounds in the extracellular space14.
Neutrophils try to digest bacteria outside their “stomack”!
The process of degranulation matters not only for bacterial killing, but also for other functions of neutrophils, such as migration and regulation. However, it is unclear, veather Vitamin C is somehow involved in that.
Weapon 3: NETosis
As it was mentioned before, pus is predominantly made of dead neutrophils. But why do neutrophils die so massively? The answer is quite simple.
Neutrophils are kamikazes!
Kamikazes is the commonly used name for Japanese soldiers, carrying out destructive suicidal attacks during the war. They loaded their aircrafts with explosives and then crashed them into enemy aircrafts or battleships. Such strategy led to massive losses in enemy forces, but it also cost kamikazes their own lives.
That is exactly what happens to neutrophils when they use NETosis.
“NET” stands for “Neutrophil Extracellular Traps”. As a response to bacteria presence, neutrophils are capable of making sticky fiber-like structures out of their own DNA and throw it in the extracellular space18,19. The neutrophil granules, that were described above, stick to these fibers and are thrown out as well. As a result, a special anti-microbial web is created, which serves two main purposes:
- The neutrophil web simply traps the bacteria, like spider web traps flies. It prevents bacteria from spreading across our bodies
- The web and the neutrophil granules create a high concentration of anti-bacterial components, that efficiently kill bacteria, that get trapped in the net
Sounds pretty cool!
Unfortunately, there is a price that comes with such a cool weapon.
- Neutrophils cannot continue to exist after throwing their own DNA out. NETosis is a single-use suicide attack for each neutrophil – just like for kamikazes
- NETosis results in a locally high concentration of toxic enzymes. While their main targets are bacteria, they are also harmful to the cells of our own body20
With this said, the process of NETosis must be tightly regulated.
Overactive NETosis can lead to consequences more severe, than the bacterial infection itself. It was shown to cause and contribute to multiple organ dysfunction20. In the lungs, excessive NETosis results in damage of alveolar epithelium and contributes to Acute Lung Injury21. Since COVID-19 is also a respiratory disease, a balance is of utmost importance here: NETosis should be used, but not overused.
Vitamin C – a regulator of neutrophil NETosis
Several studies indicate that Vitamin C is tightly involved in the prevention of excessive NETosis. It was shown, that neutrophils of Vitamin C deficient mice are generally more prone to NETosis, compared to neutrophils of mice with sufficient Vitamin C supplementation22. These differences were shown to be of utmost importance in sepsis-like conditions. Three groups of mice were compared:
- Group 1 had a sufficient amount of Vitamin C in their diet before and after the infection
- Group 2 was Vitamin C deficient but got supplemented with a high dose of the vitamin after the infection
- Group 3 was Vitamin C deficient and did not get supplemented after the infection
It turned out, that NETosus rates in the first and the second groups were similar, while mice of the third group had upregulated NETosis rates22
A similar effect of Vitamin C was shown for human neutrophils. Pre-treatment of isolated neutrophils with Vitamin C before their activation by the pathogen resulted in lower NETosis rates, compared to non-treated neutrophils22
This study indicates, that sufficient supplementation with Vitamin C is necessary to prevent excessive NETosis and subsequent tissue damage.
Humans belong to a relatively small group of mammals, unable to produce Vitamin C by themselves inside their bodies. The gene, necessary for Vitamin C production, was lost during evolution. That is why we have to rely on our nutrition as a source of Vitamin C. However, mice still have that gene. Thus, to use mice as a model organism for Vitamin C deficiency, the scientists had to damage the gene and deprive mice of the capability of producing Vitamin C
After the battle: apoptosis and clearance
As we might learn from movies about the middle ages, what happens after the battle is as important as what happens during the battle. If the dead bodies are not removed and berried – all sorts of epidemics might break out. And then you are doomed, even if you have just won your war.
Similar processes can happen in our bodies.
Debris of dead bacteria and perished immune cells, as well as still alive and feisty immune cells, need to be taken care of. For neutrophils, it means, that they have to go through a special cell death – apoptosis.
Yes, unfortunately, neutrophils never return home from war – even if the victory is on their side.
Cell death by apoptosis prevents neutrophils from committing unnecessary NETosis or initiating necrosis. Apoptosis ensures that neutrophils’ contents are not thrown out in the open to damage other cells, but are tightly packed in the membrane vesicles instead. These vesicles are called “apoptotic bodies”.
After the infection is cleared, other immune cells, macrophages, are taking up apoptotic bodies and further digest them into harmless components. If everything goes according to plan – no unnecessary harm is done to the tissue and it starts healing immediately.
Is Vitamin C important after the battle is won?
Yes, it is. It was shown by several studies, that Vitamin C deficiency inhibits neutrophil apoptosis in favor of necrosis in mice22,23. It was also discovered, that Vitamin C deficiency impairs macrophages recruitment and clearance of the inflammation site23.
Summary
We had a pleasure of going through a battlefield together with our major anti-bacterial warriors – the neutrophils! What are the conclusions that we need to take out of that adventure?
Well, let us sum it up:
- COVID-19 id caused by a virus SARS-Cov-2
- Bacterial superinfections in the case of COVID-19 are not very frequent, but they do happen
- Bacterial superinfections have a great influence on the severity and outcome of COVID-19
- Thus, not only antiviral immunity is of importance, but antibacterial immunity too
- The main warriors against bacterial infections are neutrophils – the most abundant immune cells in the blood
- Neutrophils have two main weapons against bacteria: phagocytosis and NETosis
- Vitamin C deficiency results in attenuated phagocytosis
- Sufficient supplementation with Vitamin C is necessary for protection against ROS, which is massively generated in neutrophils for phagocytosis
- Vitamin C plays an important role in preventing excessive NETosis, which would result in tissue damage
- Vitamin C deficiency leads to attenuated clearance of the site of inflammation after the bacteria are removed
- Sufficient supplementation of your body with Vitamin C is of utmost importance for your immune system
Stay healthy!
References
- https://www.sciencedirect.com/topics/medicine-and-dentistry/bacterial-superinfection
- Rynda-Apple, A., Robinson, K. M. & Alcorn, J. F. Influenza and Bacterial Superinfection: Illuminating the Immunologic Mechanisms of Disease. Infect Immun 83, 3764–3770 (2015).
- Beović, B. et al. Antibiotic use in patients with COVID-19: a ‘snapshot’ Infectious Diseases International Research Initiative (ID-IRI) survey. J Antimicrob Chemoth 75, dkaa326- (2020).
- Langford, B. J. et al. Bacterial co-infection and secondary infection in patients with COVID-19: a living rapid review and meta-analysis. Clin Microbiol Infec 26, 1622–1629 (2020).
- Arunachalam, P. S. et al. Systems biological assessment of immunity to mild versus severe COVID-19 infection in humans. Sci New York N Y 369, 1210–1220 (2020).
- Alexander, C. & Rietschel, E. T. Bacterial lipopolysaccharides and innate immunity. J Endotoxin Res 7, 167–202 (2001).
- Furtado, R. H. M. et al. Azithromycin in addition to standard of care versus standard of care alone in the treatment of patients admitted to the hospital with severe COVID-19 in Brazil (COALITION II): a randomised clinical trial. Lancet Lond Engl 396, 959–967 (2020).
- Ginsburg, A. S. & Klugman, K. P. COVID-19 pneumonia and the appropriate use of antibiotics. Lancet Global Heal 8, e1453–e1454 (2020).
- Barer, M. R. Medical Microbiology. Part 2 Infect Immun 168–173 (2012) doi:10.1016/b978-0-7020-4089-4.00029-9.
- Melzer, S. et al. Reference intervals for leukocyte subsets in adults: Results from a population-based study using 10-color flow cytometry. Cytom Part B Clin Cytom 88, 270–81 (2015).
- Pillay, J. et al. In vivo labeling with 2H2O reveals a human neutrophil lifespan of 5.4 days. Blood 116, 625–627 (2010).
- Sender, R., Fuchs, S. & Milo, R. Are We Really Vastly Outnumbered? Revisiting the Ratio of Bacterial to Host Cells in Humans. Cell 164, 337–340 (2016).
- Faurschou, M. & Borregaard, N. Neutrophil granules and secretory vesicles in inflammation. Microbes Infect 5, 1317–1327 (2003).
- Kennedy, A. D. & DeLeo, F. R. Neutrophil apoptosis and the resolution of infection. Immunol Res 43, 25–61 (2008).
- Padayatty, S. J. et al. Vitamin C as an Antioxidant: Evaluation of Its Role in Disease Prevention. J Am Coll Nutr 22, 18–35 (2003).
- REBORA, A., DALLEGRI, F. & PATRONE, F. Neutrophil dysfunction and repeated infections: influence of levamisole and ascorbic acid. Brit J Dermatol 102, 49–56 (1980).
- Levy, R., Shriker, O., Porath, A., Riesenberg, K. & Schlaeffer, F. Vitamin C for the Treatment of Recurrent Furunculosis in Patients with Impaired Neutrophil Functions. J Infect Dis 173, 1502–1505 (1996).
- Brinkmann, V. et al. Neutrophil Extracellular Traps Kill Bacteria. Science 303, 1532–1535 (2004).
- Douda, D. N., Jackson, R., Grasemann, H. & Palaniyar, N. Innate Immune Collectin Surfactant Protein D Simultaneously Binds Both Neutrophil Extracellular Traps and Carbohydrate Ligands and Promotes Bacterial Trapping. J Immunol 187, 1856–1865 (2011).
- Winterbourn, C. C. & Kettle, A. J. Redox Reactions and Microbial Killing in the Neutrophil Phagosome. Antioxid Redox Sign 18, 642–660 (2013).
- Saffarzadeh, M. et al. Neutrophil extracellular traps directly induce epithelial and endothelial cell death: a predominant role of histones. Plos One 7, e32366 (2012).
- Mohammed, B. et al. Vitamin C: A Novel Regulator of Neutrophil Extracellular Trap Formation. Nutrients 5, 3131–3150 (2013).
- Vissers, M. C. M. & Wilkie, R. P. Ascorbate deficiency results in impaired neutrophil